
Introducing Expanded Explanations!
The little box with a lot to offer...
We're pleased to report that this popular feature is now in our Pastest Med Students, PLAB 1, MRCP Part 1, MRCP Part 2, MRCP PACES, MSRA, MRCS PART A, MRCPCH FOP/TAS, MRCPCH AKP and MRCGP (AKT) online resources.
At Pastest, we're always listening to our users - and this feature was requested by many students and junior doctors in recent focus groups.
Now, when you answer a question, you can review a new Expanded Explanation of the question topic, as well as our dynamic explanations for each answer choice.
Each Expanded Explanation contains subsections so that you can quickly navigate to the information you need. These can include a Topic Overview, Clinical Presentation, Differential Diagnosis, Diagnosis/Investigation, Management, Prognosis, and External Links.
Take a look at our example explanation below, to get a feel for the depth of content that's now at your fingertips. This is just one of hundreds of explanations displayed after you answer a question. Look out for it on the right-hand side of the window, or below the answer explanations if you're on a mobile device or using our app.
Expanded Explanation
Psoriasis
Jump to:
Overview
Key facts
- An immune-mediated, chronic, multi-system inflammatory disease:
- primarily associated with hyperproliferation of keratinocytes in the epidermis
- often follows a relapsing/remitting course
- plaque psoriasis is the most common form (up to 90% of all psoriasis cases), associated with well-defined, red, disc-like plaques covered by white/silver scales
- commonly affected areas include the elbows, knees, back and scalp.
- Approximately 30% of patients have associated joint involvement.
- Treatment depends on severity, location of disease and the impact on the individual.
Epidemiology
- Psoriasis occurs in 1-2% of the United Kingdom’s population.
- It affects both genders equally.
- It can occur at any age, with peak age ranges of 16-22 and 57-60 years old.
- It is uncommon in childhood.
Aetiology
- Aetiology is unknown but multiple genetic factions in combination with environmental factors are thought to be important.
- 30% of patients with psoriasis have an affected first-degree relative.
- If both parents are affected, the risk of a child developing psoriasis is 75%.
- There are several psoriasis-susceptibility gene loci (eg PSOR1) and genes involved in interleukin (IL)-23 signalling, modulation of T-helper (Th)-2 immune responses (IL-4, IL-13) and activated B-cell (NF-kB) signalling have been identified.
Pathophysiology
- The understanding of psoriasis has moved from one of a hyperkeratotic disorder of keratinocytes to a dysregulation of the immune system mediated by cytokines.
- Th-1, Th-17 and Th-22 cell populations are expanded and stimulated to release inflammatory cytokines, including IL-17, IL-22 and tumour necrosis factor alpha (TNF-a).
Clinical Presentation
- Chronic plaque (90% of cases):
- well-defined, red, disc-like plaques covered by white/silver scale, which classically affects extensor surfaces of elbows, knees; and the scalp.
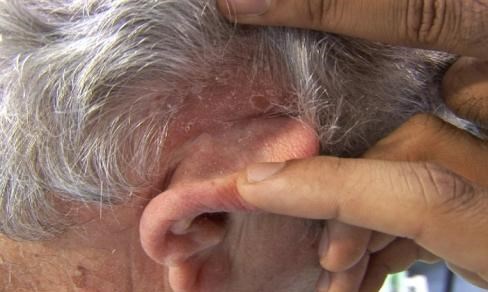
Scalp psoriasis
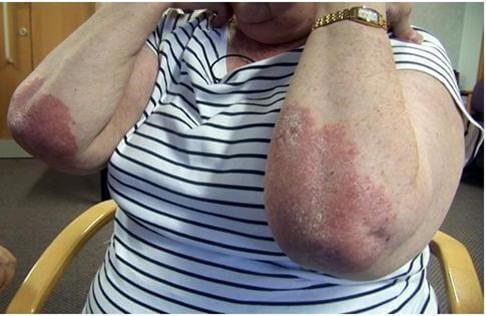
Plaque psoriasis on the extensor surface of the elbow
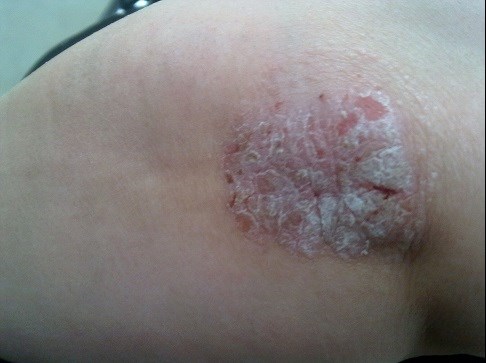
Image Source: https://commons.wikimedia.org/wiki/File:Psoriasis_in_elbow.jpg
Plaque psoriasis
- Pustular (generalised pustular):
- sheets of small, sterile yellow pustules on a red background.
- This presentation may be accompanied by systemic symptoms and progression to erythroderma.
- Erythrodermic:
- confluent areas affecting most of the skin surface.
- Nail involvement in psoriasis:
- onycholysis, pitting and subungual hyperkeratosis.
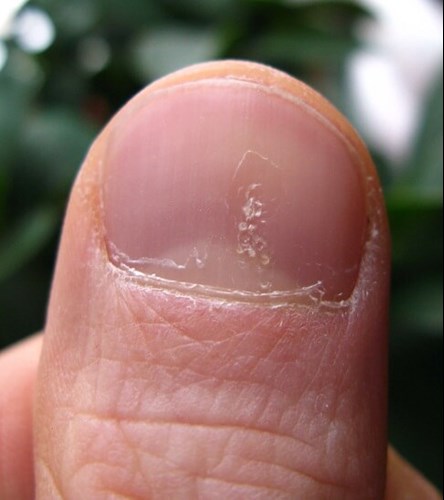
Image Source: https://upload.wikimedia.org/wikipedia/commons/b/b3/Luszczyca_paznokcia.jpg
- Pustular (palmoplantar pustulosis):
- yellow/brown sterile pustules and erythema on palms/soles
- strongly associated with smoking
- often seen in middle-aged women.
- Guttate:
- an acute eruption of drop-like lesions, often following a streptococcal sore throat.
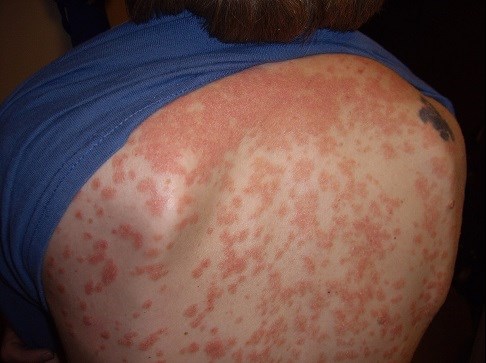
Image Source: https://commons.wikimedia.org/wiki/File:Guttate_psoriasis.jpg
- Flexural:
- affects axillae, sub-mammary areas and the natal cleft
- lesions are often smooth, red and glazed in appearance.
Exacerbating Factors:
- Trauma: Koebner phenomenon (development of disease in areas of trauma).
- Infection: for example, streptococci (guttate psoriasis).
- Human immunodeficiency virus (HIV): psoriasis is more common in patients with HIV; severity may dwindle in later stages.
- Endocrine: psoriasis tends to improve during pregnancy and deteriorate in post-partum period.
- Drugs: beta-blockers, lithium, antimalarial interferon, and withdrawal of oral steroids may exacerbate psoriasis.
- Alcohol
- Stress
- Smoking: smoking is associated with increased incidence and severity.
- Ultraviolet (UV) light: although most patients find UV light beneficial, a small number experience UV light associated flare-ups.
Differential Diagnosis
- Differential diagnoses for psoriasis include:
Diagnosis
- Diagnosis is mainly clinical.
- Specialist advice should be sought if there is diagnostic uncertainty.
- The patient should then be assessed for:
Management
Non-pharmacological
- Offer support and information tailored to suit individual needs and circumstances so that they can confidently understand the following:
- their diagnosis and treatment options
- relevant lifestyle risk factors
- when and how to use prescribed treatments safely and effectively
- when and how to seek further general or specialist review
- strategies to deal with the impact of psoriasis on physical and social wellbeing.
- Refer for specialist advice if there is:
- diagnostic uncertainty
- severe or extensive psoriasis and/or acute guttate psoriasis
- generalised pustular psoriasis or erythroderma (needs same day specialist assessment and treatment)
- uncontrolled symptoms despite topical therapy
- the patient is a child or young person
- a major impact on the patients physical, social or psychological wellbeing.
Pharmacological
First-line Treatment - Topical Therapy:
- Coal tar preparations:
- crude coal tar can be useful in thick plaque psoriasis.
- Dithranol:
- synthetic derivative of anthracene
- effective but needs accurate applications as it can burn the surrounding skin and stain clothing.
- Vitamin D analogues:
- calcipotriol cream/ointment
- calcipotriol with betamethasone.
- Taraztoene:
- a topical retinoid for plaque psoriasis.
- Topical steroids:
- used alone or in combination or with other topicals for face, genitalia, flexures, hands, feet, and scalp
- steroid strength may vary according to severity and body site.
Second-line Treatment:
- Offer phototherapy or non-biological systemic agents when:
- topical therapy alone is unlikely to control disease (eg > 10% body surface area (BSA) or nail disease), and
- disease has a significant impact on physical, psychological and/or social wellbeing, or
- there is significant functional impairment, or
- there are high levels of distress (including severe nail involvement, high-impact site of disease).
- Non-biologics may be indicated when phototherapy is ineffective; however, it cannot be used if there is a rapid relapse following phototherapy.
Phototherapy:
- Ultraviolet B-rays (UVB) narrowband – well established and effective.
- Psoralen and ultraviolet A radiation (PUVA) use necessitates the need for protective eyewear and is associated with an increased risk of skin cancers.
Non-biological systemic treatment
- Risk and/or benefits must be weighed up when considering prescribing the following:
- methotrexate is a first-line non-biological systemic treatment. It blocks DNA syntheses by inhibiting dihydrofolate reductase and is administered once-weekly either orally or by subcutaneous injection. Risks of anaemia/pancytopenia/nausea are reduced with folic acid supplementation. There is a risk of liver fibrosis with long-term use. The serological marker for fibrosis procollagen-3 N-terminal peptide (P3NP) should be measured 3-monthly
- ciclosporin is a first-line non-biological systemic treatment where rapid/short-term disease control is required, eg a flare/palmar pustulosis, or when conception is being considered. It inhibits T-lymphocyte transcription of IL-2. Side-effects of ciclosporin include renal toxicity and hypertension
- retinoids, for example, acitretin, used alone and/or in combination with UVB/PUVA, if methotrexate or ciclosporin is not appropriate or ineffective. Should be avoided in women with childbearing potential due to teratogenic affects. Mucocutaneous side-effects are common, triglyceride level elevation can occur and should be monitored.
Third-line Treatment - Biologic Agents:
- Biologics are considered for patients with severe disease. Strict eligibility criteria are in place, indications include:
- no response to standard first- and second-line treatments
- intolerance to other standard first- or second-line treatments
- other treatments contraindicated
- severe life-threatening disease
- for biological treatments, severity scores such as psoriasis area and severity (PASI) score and dermatology life quality index (DLQI) must be at least ten.
- Currently, the National Institute for Health and Care Excellence (NICE) approve biologic target TNF-α or the interleukin pathways:
- etanercept: human protein fusion of the TNF receptor that acts as a TNF-α inhibitor. Delivered via subcutaneous injection
- adalimumab: a human monoclonal antibody that binds to TNF-α. Delivered via subcutaneous injection
- infliximab: a chimeric monoclonal antibody that binds to TNF-α. Delivered via infusion
- ustekinumab: a human monoclonal antibody that targets IL-12 and IL-23. Delivered subcutaneously.
- Other biologics are currently under development.
Prognosis
- The condition often has a relapsing/remitting course and is associated with significant functional, psychological, and social morbidity for many patients.
- As a systemic condition, inflammatory processes involved are associated with the development of numerous co-morbidities as well as reduced life expectancy.
- Associations with psoriasis:
- major adverse cardiac events (MACE): studies show that psoriasis sufferers have a 53% increased incidence of MACE (myocardial infarction, stroke, cardiac death). Risk is also increased due to the strong association of the metabolic syndrome (hypertension, obesity, diabetes, dyslipidaemia) with psoriasis
- venous thromboembolism: especially with severe psoriasis
- arthropathy: psoriatic arthritis occurs in approximately 20% of patients with skin psoriasis. There are several different forms including distal interphalangeal joint disease, arthritis mutilans, sacroiliitis, psoriatic spondylitis
- gout: due to deposition of urate crystals
- malabsorption: due to associations with Crohn’s disease and ulcerative colitis
- lymphoma: approximately threefold increased incidence with psoriasis
- skin malignancy: non-melanoma type.
Other relevant information
Skin disorder | Causes of nail changes associated with skin disorders |
Psoriasis | Onycholysis, nail pitting, hyperkeratosis, pustule and occasional loss of nail |
Fungal | Discoloration, onycholysis and thickening of the nail |
Bacterial | Usually due to staphylococcal infections – pseudomonas infections give nails a green discolouration |
Lichen planus | Nail changes occur in 10% of cases, with thinning of nail plate and longitudinal linear depressions – occasionally destruction of the nail (pterygium) |
Alopecia areata | Pitting, thickening and ridging of the nail (sandpaper nail) are seen |
Dermatitis | Coarse pits, cross-ridging and onycholysis may be seen |
- Causes of the Koebner phenomenon:
- psoriasis
- lichen planus
- vitiligo
- viral warts
- molluscum contagiosum.
- Causes of erythroderma:
- psoriasis
- eczema
- mycosis fungoides
- adverse drug reactions
- underlying malignancy
- pityriasis rubra pilaris.
Links to NICE guidelines/CKS
NICE guideline – Psoriasis: assessment and management
- 09 Dec 2021
- News